Treating IBD: Simple Steps to Manage Crohn’s & Ulcerative Colitis
If you’ve been told you have inflammatory bowel disease (IBD), the first thing to know is that you’re not alone and there are plenty of tools to keep symptoms in check. Most people think IBD means a life‑sentence of pain, but with the right meds and daily habits you can stay active, enjoy meals, and avoid flare‑ups.
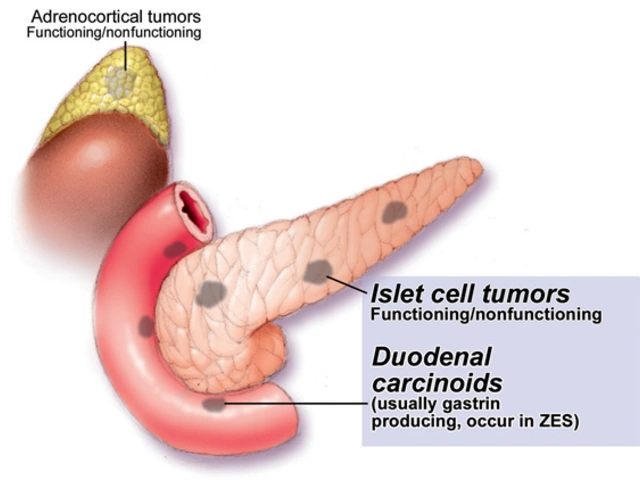
IBD covers two main conditions – Crohn’s disease and ulcerative colitis. Both involve inflammation in the gut, but they affect different areas. Crohn’s can hit any part of the digestive tract, while ulcerative colitis stays limited to the colon. Understanding which one you have helps your doctor pick the right treatment plan.
Medication Basics You Should Know
The first line of defense is usually 5‑aminosalicylic acid (5‑ASA) drugs like mesalamine. They work on mild inflammation and are taken orally or as a rectal foam. If symptoms keep coming back, doctors often add steroids for short bursts – think prednisone or budesonide. Steroids calm flare‑ups fast but aren’t meant for long‑term use because of side effects.
When the disease steps up a gear, immunomodulators such as azathioprine or methotrexate come into play. These medicines dial down the immune system so it doesn’t attack your gut as hard. They take weeks to show results, so patience is key.
The newest class is biologics – injectable or IV drugs that target specific inflammatory proteins. Examples include infliximab, adalimumab, and ustekinumab. Biologics have changed the game for many patients, shrinking hospital visits and letting people lead normal lives. Your doctor will run blood tests to make sure you’re a good candidate before starting.
Everyday Habits That Ease Symptoms
Medication does most of the heavy lifting, but daily habits can tip the balance between calm and flare‑up. First up: food. No single diet cures IBD, but many people feel better by limiting high‑fiber foods during active phases, steering clear of spicy or greasy meals, and watching out for lactose if they’re sensitive.
Keeping a simple food journal helps you spot triggers. Write down what you eat, how you feel afterward, and any symptoms that show up. Over time you’ll see patterns – maybe coffee or certain nuts are the culprits.
Staying hydrated is another must‑do. Diarrhea can drain fluids fast, so aim for at least eight glasses of water a day. If you’re on steroids, add potassium‑rich foods like bananas to balance electrolytes.
Stress doesn’t cause IBD, but it sure makes symptoms worse. Try low‑effort stress reducers: short walks, breathing exercises, or a quick 10‑minute meditation app. Consistency beats intensity – doing something small every day adds up.
Exercise works like a gentle anti‑inflammatory. Low‑impact activities such as swimming, cycling, or yoga keep joints happy and improve gut motility without jarring the abdomen.
Lastly, don’t skip follow‑up appointments. Your doctor monitors blood work, colonoscopy results, and how well meds are working. If you notice new symptoms – sudden weight loss, fever, or severe abdominal pain – call them right away.
Putting these pieces together – the right medication mix, a food log, hydration, stress control, and regular check‑ins – gives you a solid plan to treat IBD. It won’t magically erase the disease, but it puts you in charge of how often it shows up in your life.

- Apr 29, 2023
- Posted by Cillian Osterfield
The Role of Mesalamine in Treating IBD-Related Joint Pain
As a blogger who deals with health topics, I've recently come across the role of Mesalamine in treating IBD-related joint pain. IBD or Inflammatory Bowel Disease often leads to joint pain, causing discomfort and affecting the quality of life of patients. Mesalamine is an anti-inflammatory medication that has shown to be effective in managing this pain. By reducing inflammation in the gastrointestinal tract, it also alleviates the inflammation in joints, providing much-needed relief to IBD sufferers. It's great to know that there's a medication available that can help improve the lives of those dealing with IBD-related joint pain.
Categories
- Medications (79)
- Health and Wellness (73)
- Health and Medicine (31)
- Pharmacy Services (13)
- Mental Health (10)
- Medical Research (3)
- Health and Career (2)
- Business and Finance (2)
- Health Information (2)
Latest Posts
Tag Cloud
- generic drugs
- online pharmacy
- side effects
- drug interactions
- prevention
- management
- medication safety
- generic medications
- medication adherence
- bioequivalence
- treatment
- azathioprine
- dietary supplement
- generic vs brand
- smoking
- heart disease
- generic substitution
- therapeutic equivalence
- role
- panic disorder
©2026 heydoctor.su. All rights reserved